From record-breaking enrollments to exciting technology advancements, 2025 was a year of growth and success for Ritter Insurance Marketing agents and staff!
Below, we’re covering the highlights as we recap the Ritter’s State of the Senior Market for 2026. You can watch Craig Ritter’s full presentation here:
Reviewing Ritter’s 2025 Accomplishments
Behind the scenes, Ritter experienced another amazing year with increased agent-assisted enrollments and new carrier additions!
2025 Agents’ Sales Results
Medicare Advantage (MA) production for 2025 increased 27 percent, totaling 214,564 enrollments!
With Medicare Supplements, Ritter saw an 11 percent decrease in premium production, totaling $44,698,700, throughout the full plan year.
Finally, with Medicare Part D, we saw a decrease of 81 percent in enrollments from last year, for a total of 9,634 enrollments.
2026 AEP Sales Results
Our 2026 Annual Enrollment Period (AEP) saw some huge growth in MA plans. Our total number of AEP-specific MA enrollments was up an impressive 20 percent from the 2025 AEP, totaling 120,866.
Our Part D enrollments were down 21 percent compared to the previous AEP, for a total of 5,197.
In total, our enrollments for the 2026 AEP were 126,063. We couldn’t be prouder of this accomplishment, and it would not have been possible without our hardworking and devoted agents and staff!
Our grand total of enrollments for the 2026 AEP was 126,063.
New Carrier Partnerships
In 2025, we added five Medicare carriers — The Health Plan, Peak Health, Kaiser Permanente, Blue Cross Blue Shield of Michigan, and Gold Kidney Health Plan!
Two Affordable Care Act (ACA)/individual health insurance carriers — Blue Cross Blue Shield of Michigan, and Molina Healthcare of New York became available through Ritter as well!
Technology Advancements
This past year, technology enhancements were made to help make our tools and resources the best they possibly can be for our agents.
Ritter staff continues to work within Integrity to enhance its technology. Ask Integrity is becoming a more powerful virtual assistant for agents with more plan insights.
Within IntegrityCONNECT, Ask Integrity can quickly:
- Summarize client details
- Recall past appointments or call notes
- Provide plan insights or recommendations through simple prompts
IntegrityCONNECT continues to see CRM enhancements as well. Be on the lookout for its new insurance client appointment scheduler coming soon!
Register with Ritter to start using Ask Integrity and other tools! This is your opportunity to work smarter not harder!
Advocacy in Action
Our CEO, Craig Ritter, has been actively advocating for agents and brokers at the federal level.
Over the past year, he has made multiple trips to Washington, D.C. to meet with legislators and officials at CMS, sharing feedback from the field and highlighting the important role agents and brokers play in helping consumers navigate health coverage decisions.
During these discussions, Craig has advocated for several policy improvements such as:
- Changing Scope of Appointment to Scope of Relationship, creating a one-time, evergreen agreement between the agent and client. The client would have the power to designate when the scope expires at signing.
- Excluding licensed, contracted, certified, and appointed agents from the TPMO definition and removing the TPMO disclaimer.
- Keeping health plan commissions fixed from October 1 through AEP, with required advance notice of 30 to 60 days for any changes afterward.
- Protecting renewal commissions, ensuring agents continue to receive them as long as the member stays in the plan and the agent remains certified and ready-to-sell.
- Providing dual-eligible beneficiaries at least one lock-in Special Enrollment Period to enroll in a D-SNP, regardless of HIDE or FIDE plan structures.
Craig has also been working to help amend the Independent BROKERS TIME Act of 2025, introduced by Mike Rounds, which aims to address regulatory burdens affecting independent agents.
Plan Year 2025 Medicare Enrollment Stats
In 2025, MA plan enrollment continued to rise but at a slower growth rate than previous years.
Growth by Plan Type
Individual MA enrollments were up three percent as of February 1, 2026! UnitedHealthcare once again emerged as the MA market leader, with around 7.7 million enrollees at the beginning of February 2026.
Humana trailed UnitedHealthcare, taking second place, and CVS/Aetna trailed both, taking third. Devoted Health saw notable growth in MA enrollments, with a 120 percent positive year-over-year change. For reference, Humana grew 20 percent, while Centene, Cigna, CVS/Aetna, Elevance, and UnitedHealthcare all saw decreases in enrollments over the past year.
Devoted Health saw notable growth in MA enrollments, with a 120 percent positive year-over-year change.
Regional carriers like Healthfirst, Excellus, and Clover all grew year-over-year from 2025 to 2026 as well, showing the importance of offering both regional and national insurance carriers to clients.
Special Needs Plans (SNPs) had a 12 percent year-over-year growth, proving they are a rising MA product! Try adding SNPs to your portfolio to help even more clients.
Additionally, during AEP, traditional HMOs outperformed local PPOs again.
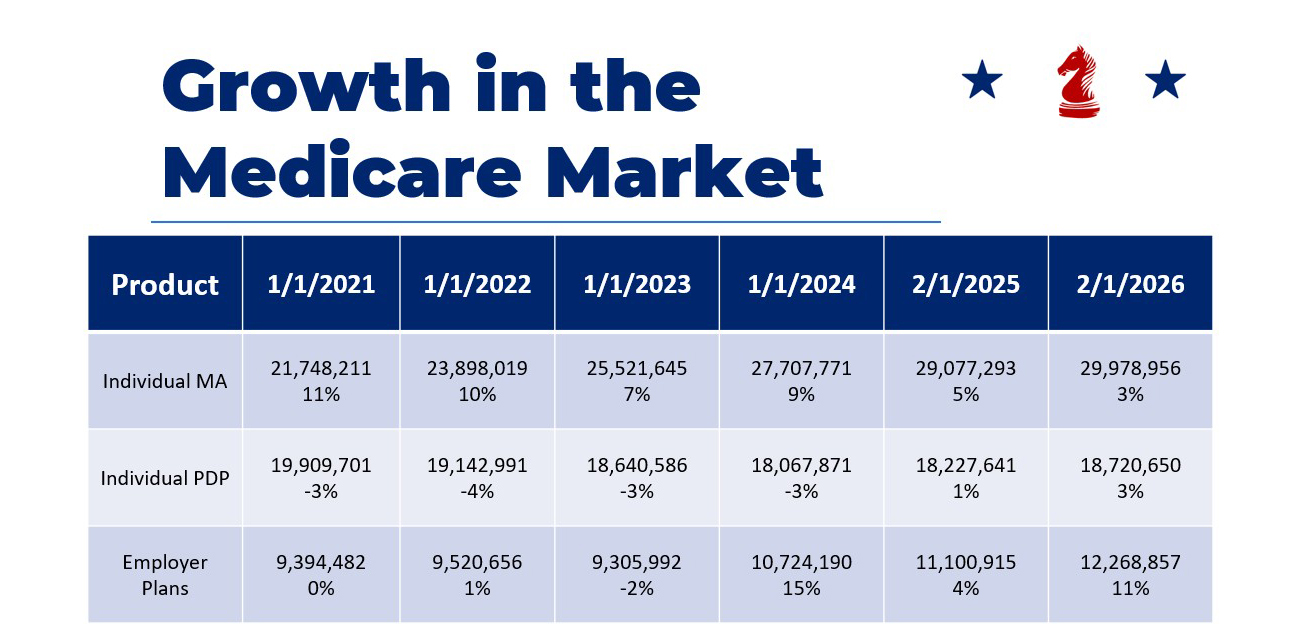
Looking at prescription drug plans, enrollment increased by about three percent, which is an improvement from the one percent increase from 2024 to 2025. Humana saw the most growth over the past year, but Wellcare saw some growth as well.
Growth by State
Texas had the highest number of enrollments — 35,791. Florida and North Carolina followed with 29,400 and 26,203 enrollments, respectively.
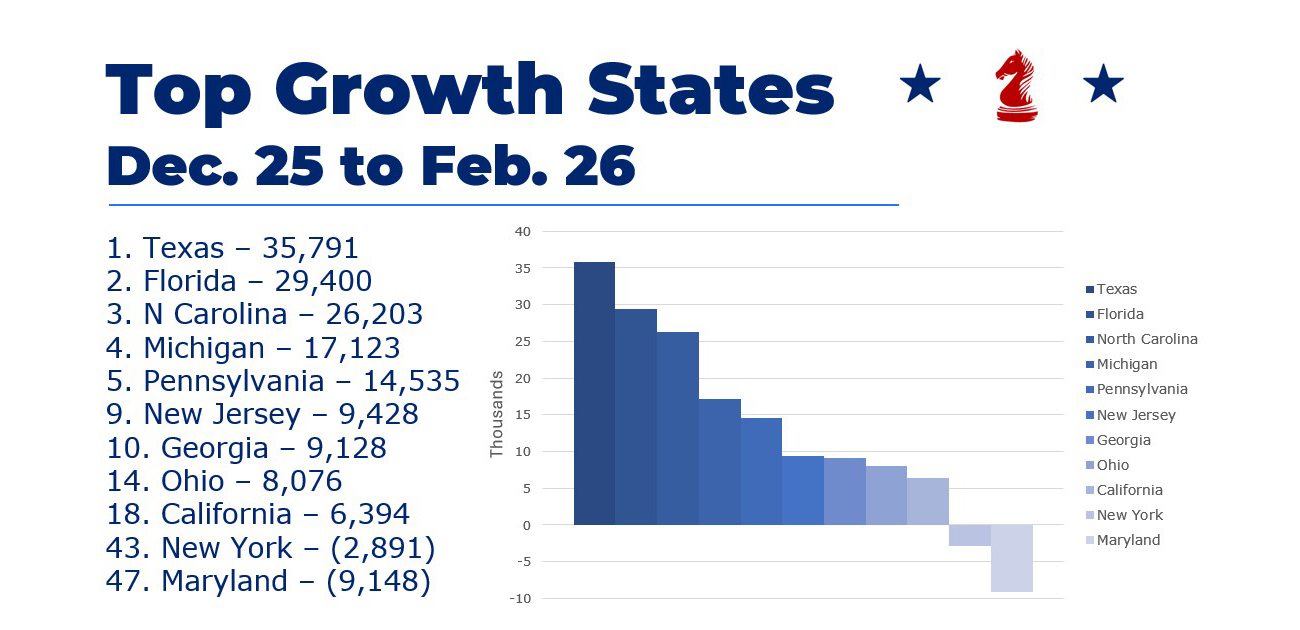
In the recording of the address, we dive deeper into carrier growth per state, so check that out if you want additional localized insight!
Medicare Regulation and Legislation & Industry Trends
The Medicare landscape has been changing over the past year, and we’ll see changes continue throughout PY2026. Here’s what you should know about.
Projecting 2027 Commissions
CMS officially releases MA & Part D broker commissions around the end of May. Based on CMS’ 2027 Advance Notice and the 4.97 percent effective growth rate, we expect Medicare Advantage maximum broker commissions to increase five percent from 2026 to 2027.
Below is what the figures would look like.
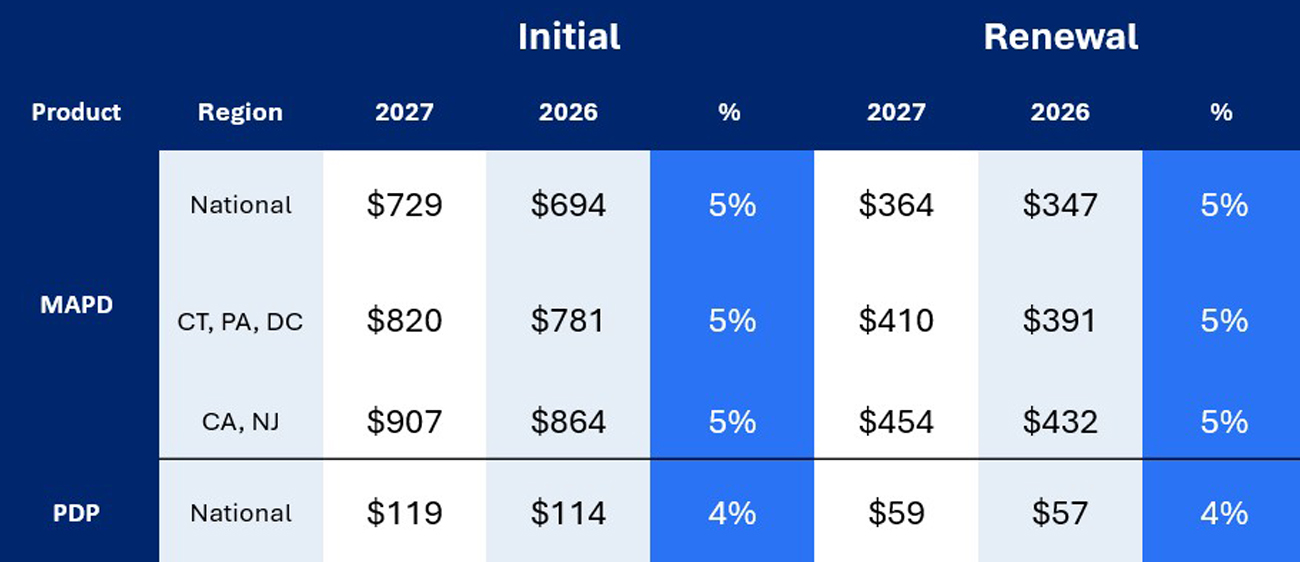
Note: These are Craig Ritter’s projections and not the official maximum broker commissions for 2027.
CY2027 Part D Standard Benefit
In 2027, the annual true out-of-pocket costs will be capped at $2,400 for those enrolled in Medicare Part D. This is an increase of $300 from 2026. The deductible will be $700, which is an $85 increase from 2026.
The defined Part D prescription drug coverage benefits will consist of three phases:
- Deductible — The enrollee pays 100 percent of their covered prescription drug costs (GCPDC) until the deductible of $700 for CY 2027 is met.
- Initial coverage — The enrollee pays 25 percent coinsurance for covered Part D drugs until the out-of-pocket cost hits $2,400.
- Catastrophic — The enrollee pays no cost-sharing for covered Part D drugs.
Enrollees will also have the option to pay out-of-pocket prescription drug costs via capped monthly payments.
New Marketing Requirements
Several 2027 MA & Part D Final Rule changes could impact how agents conduct events, handle call recordings, and use required disclaimers.
For educational events, the proposed updates would:
- Remove the current 12-hour waiting period between educational and marketing events.
- Allow agents to collect Scope of Appointment (SOA) forms during educational events.
- Shorten the required retention period for recorded sales calls from 10 to six years.
In addition, changes to the TPMO disclaimer would remove the requirement to reference SHIP.The disclaimer would still need to be read during calls, but it would no longer be required within the first minute of the conversation.
Medicare Supplement Birthday Rules
Birthday rules have been driving Medicare Supplement rates and commissions changes.
In select states, policyholders have a window of time around their birthday each year when they can switch to a Med Supp with slightly different or the same benefits, depending on the state.
Below you can see which states are participating or proposing to:
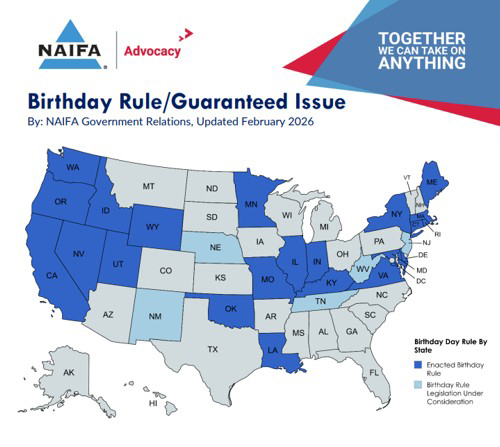
If your client lives in one of these states and is unhappy with their coverage, there’s no point in waiting until AEP if their birthday comes first!
Part D Carrier Actions Due to Market Pressure
As a result of the IRA and Part D redesigns, there has been a massive increase in upfront payments and risk transfer to insurers.
We’ve seen also dramatic consolidation in the Part D market:
- The number of Part D plans offered by carriers decreased by almost 50 percent since 2024.
- Market share of the top two carriers increased from 57 percent to 64 percent.
This margin pressure and consolidation has led to reduced commissions and zero commissions for agents.
MA Carrier Actions Due to Market Pressure
From 2023 to 2025, Medicare Advantage plans experienced an estimated $95 per-member headwind driven by multiple factors.
The share of beneficiaries enrolled in 4-star or higher plans declined significantly, from about 89% to 64%, while MA funding was negative in both 2024 and 2025. At the same time, The CMS-HCC Risk Adjustment Model (v28) contributed to an additional three percent revenue decline between 2023 and 2025, which further tightened margins for carriers.
These pressures have affected beneficiary behavior and carrier sales strategies. Disenrollment has increased sharply, rising from roughly one percent of MA members annually between 2018 and 2024 to about seven percent (1.8 million members) in 2025 and an estimated 10% (2.8 million members) in 2026, with even higher rates among non-SNP plans.
In response, carriers have begun taking steps to better control enrollment and profitability. While plans historically boosted spending marketing dollars to drive sales, the past two AEPs have seen the opposite approach, including limiting third-party enrollment platform access (such as Sunfire and Connecture) and removing commissions on certain new sales.
These actions reflect a broader shift toward managing growth more carefully as plans adjust to the evolving MA landscape.
Broker Compensation Protection Updates
Industry groups are working with NAIFA to push for greater transparency around broker commissions. There are a few actions you can take to keep earning commissions as well.
NAIFA’s Proposal
Currently, health plans submit a range of commissions in their CMS bids, often from $0 to the CMS maximum, rather than a specific amount.
Because these filings typically include a single marketing budget that covers multiple activities, actual commissions can vary widely.
NAIFA is proposing CMS require a reasonable floor within the filing range, so brokers receive more consistent compensation. If adopted, the change would likely not take effect until PY 2028 at the earliest.
Thanks to Ritter, if you decide to join NAIFA, you’ll receive 50 percent off your dues with a special Medicare Collective rate, just $360 annually or $30 a month.
Preparing for Market Pressure
Brokers can prepare by strengthening client relationships, expanding their MA carrier portfolio, certifying early, and staying flexible instead of relying on a single “go-to” plan.
Engaging clients early to gather SOAs, drug lists, pharmacies, and provider information can also help streamline enrollment.
Diversifying Revenue
As benefits potentially tighten, brokers may profit from introducing ancillary products such as hospital indemnity, cancer, dental, vision, and hearing coverage.
Expanding into life, wealth, and broader health solutions can also help increase revenue per insurance client.
Leveraging technology for plan comparisons and enrollment can further improve efficiency and support growth. You can do all of this with IntegrityCONNECT! Easily view plan options and when it’s time to enroll clients, your saved information will automatically fill in.
When you set up your own PlanEnroll website, clients can also compare plans that you offer from the comfort of their own home.
Ritter’s CEO, Craig Ritter, wants to be your advocate when it comes to the Medicare space and aims to emphasize an agent’s role in the enrollment process.
We’re excited to see what’s in store for the future of Medicare, and we hope to keep helping agents find success in the business!
Unable to attend this year’s State of the Senior Market address? You can watch the recording whenever you’d like!
If you aren’t yet a Ritter agent, register with us today to start selling smarter than ever with an excellent partner by your side.









Not affiliated with or endorsed by Medicare or any government agency.
Share Post